Type 1 diabetes can strike anyone, regardless of how old they are or the size of their waistline. The disease prevents the body from producing enough insulin to regulate a person’s blood glucose level, meaning the amount of sugar in the blood is too high.
People with diabetes need to take several small samples of blood throughout the day, and perform daily injections to help control their blood glucose levels. A finger prick test requires using a minute needle to break the skin to obtain a small sample of blood which is placed into a reader on a test strip. The resulting reading is the blood glucose level, and this helps the diabetic to manage the disease.
However, two new methods that monitor the levels of glucose in the interstitial fluid (the fluid found in between cells) have come into the foreground, working alongside the finger prick test.
Flash Glucose Sensing
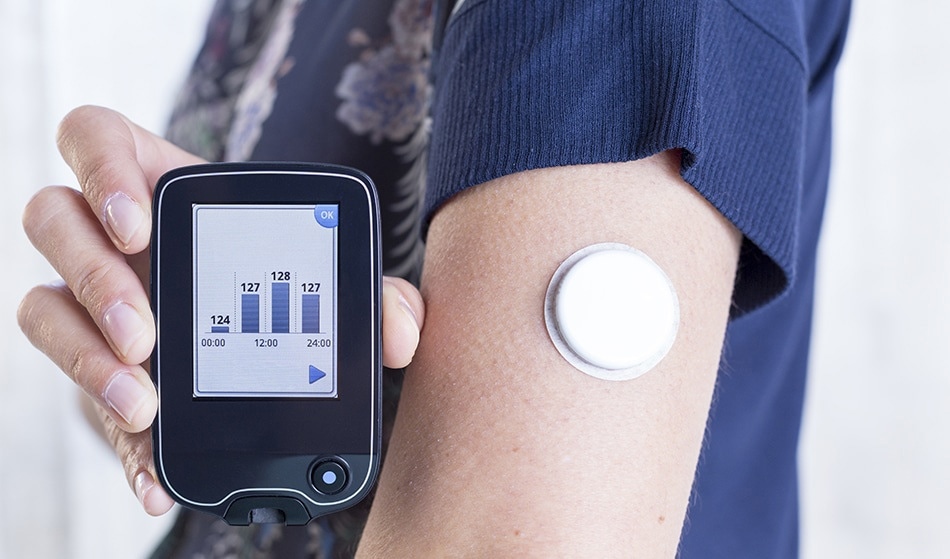
Click and Photo / Shutterstock
Flash glucose sensing scans blood glucose levels via a sensor around the size of a £2 coin, which is placed on the back of a person’s arm. A probe sits just under the skin and measures the amount of glucose in the interstitial fluid. The sensor is ‘flashed’ with a scanning device, which then displays a blood glucose level reading, a graph detailing blood glucose levels for the previous eight hours, as well as a directional arrow to show if levels are increasing or decreasing. This allows the user to see how their blood glucose levels change over time – even while they are asleep.
Although evidence shows that this method can help people with type 1 diabetes manage their condition and keep them healthy, currently only one flash glucose sensing device is available on the NHS, and whether patients are entitled to one is a bit of a postcode lottery.
Continuous Blood Glucose Testing
Sensors that record glucose levels continuously allow the user to see how fast and in what direction their glucose levels are going. A tiny glucose-sensing device is placed just under the skin, usually around the abdomen or upper buttock area, which measures the level of glucose in the interstitial fluid every 10 seconds. This is then converted into an electrical signal which represents the amount of sugar in the blood. A small transmitter attached to the sensor then sends a signal to an insulin pump or monitor.
Finger prick tests are still required to help calibrate the monitor, which records the average glucose values every five minutes for up to 72 hours, at which point they can be downloaded, reviewed and subsequently adjusted.
What’s Best?
Neither continuous blood glucose testing nor flash glucose testing are meant to replace monitoring with finger prick tests. They are both ideal for identifying fluctuations and trends that might be missed with finger prick test measurements, allowing a user to take action to avoid severe high or low blood sugar levels. However, their readings tend to lag between five and 15 minutes behind actual levels found in the blood, so finger prick tests must still be taken - particularly when exercising or if feeling unwell.
The Future
Romaset / Shutterstock
Teams across the globe are investigating the use of sensors to monitor blood glucose. Researchers from the University of Bath have developed a new kind of technology that could see the end of finger prick blood tests for diabetics; a wearable sensor that measures glucose levels through the skin. Like other sensors, it draws glucose from the interstitial fluid, this time between cells across hair follicles retrieved via an array of miniature sensors using small electrical currents. The result is regular, as clinically relevant glucose measurements can be sent directly to a user’s phone or monitor.
Researchers from the University of Glasgow are exploring the possibility of using wearable sensors to measure the pH of sweat, which they say could also eliminate the need for the finger prick test. Much of the physiological information in sweat is the same as the information contained in blood, and it is hoped that its diagnostic uses will eradicate the need for diabetics to break the skin to administer the test. The team hope to expand the patch’s capabilities to measure glucose, ammonia and urea, all on a sensor the size of a postage stamp.
Although many of these sensors do not directly test blood, they are a useful tool for monitoring glucose levels in the blood of diabetics. In the future, sensors such as these may eliminate the need for quite so many finger prick tests.
References and Further Reading
Disclaimer: The views expressed here are those of the author expressed in their private capacity and do not necessarily represent the views of AZoM.com Limited T/A AZoNetwork the owner and operator of this website. This disclaimer forms part of the Terms and conditions of use of this website.